Managing benefit plans is time-consuming and subject to human error, which can affect performance and regulatory compliance. A firm alignment between business and IT leads to efficient benefits plan management. With a suite of tools, such as those from GalaxE Solutions, you can automate and streamline benefit plan capture, benefit translation, and claims certification. This creates a true end-to-end solution for benefits management so you can work smarter.
The Gx solution is a customizable hybrid of core automation technology enhanced with your business knowledge and processes. Your organization will experience end-to-end benefits management with our comprehensive solution suite: GxCare™, GxClaims™, and GxSelfService™. This powerful set of tools consolidates and automates a once fragmented and inefficient benefits management process, creating organization and structure. Real-time interfaces speed up the process from days to minutes, allowing organizations to dig deeper and analyze many what-if scenarios. GalaxE’s solutions meet regulatory and compliance requirements while achieving speed to market, accuracy, and agility.
A dual interface allows for backward compatibility, so clients can automatically import benefits components including copay, coinsurance, tiers, drug lists, and formularies, as well as plan building, review of plans, quality checks, and audits. The features of quality assurance through criteria building, claims selection, claims submission, claims analysis and reverse tracker are automated and accurate.
Let’s take a look at each tool in the suite:
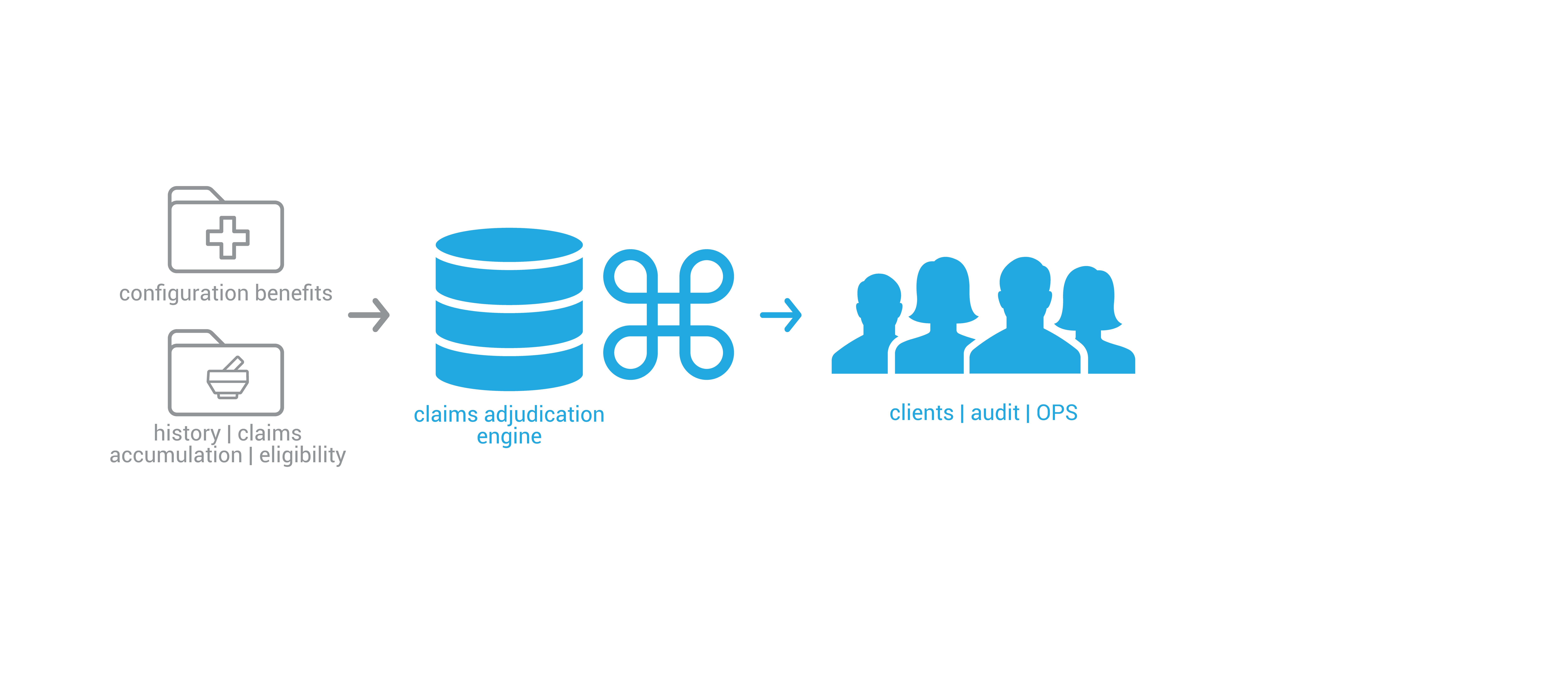
GxCare™ facilitates medical and pharmacy benefits management by collecting, interpreting, and analyzing plan data. It automates benefits plan management for intake, modeling, and cataloging, streamlining the process. Designed to be scalable and flexible with rules-driven translations and benefit loading, GxCare™ provides greater accuracy, higher efficiency, and enhanced speed to market.
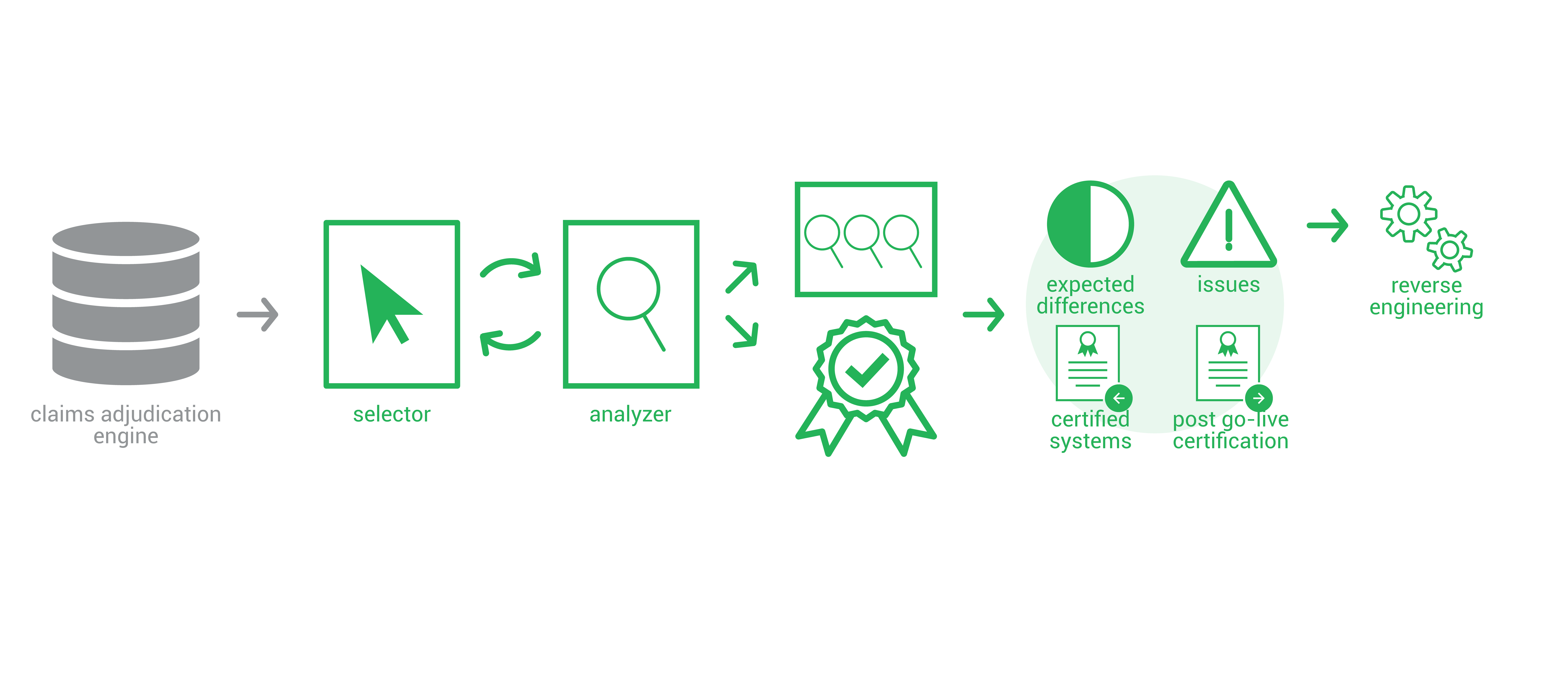
GxClaims™ brings automated innovation to the claims process to validate claim behavior and increase efficiency in identifying the root cause for unexpected claim outcomes. Audit-trail outputs help to define, test, and validate claim behavior within an adjudication system for demographic and/or clinical applications. GxClaims™ offers demographic and clinical selection, benefit plan certification, claim adjudication analysis, and an integrated defect tracking process.
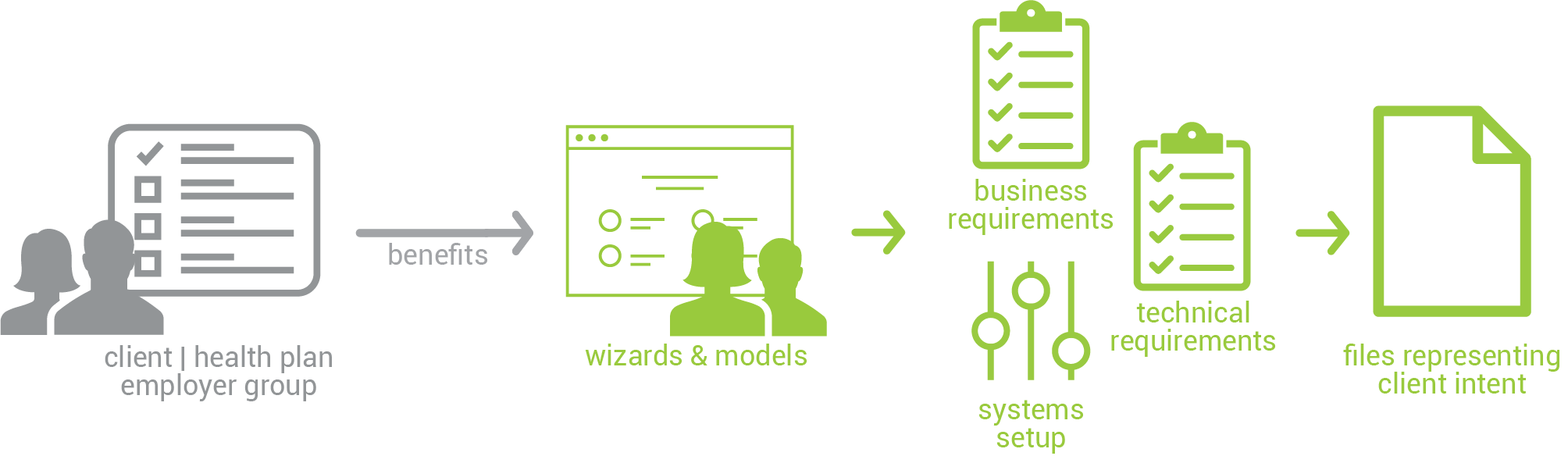
GxSelfService™ is a client benefit plan intent capture portal to onboard new clients. The web-based system is configurable, customizable, and easy to use. GxSelfService™ delivers greater transparency to customer information, reduces communication errors, and decreases operational costs. Key features include a web-based interface, direct capture of intent, end-to-end traceability, and integration.
Automating your benefit plan management, maintenance, and migration can increase productivity and impact your bottom line. GalaxE built its proprietary benefit management system from the ground up, recognizing the need to ensure an integrated, seamless process. By using the concept of code coverage for software, benefits coverage can be thoroughly reviewed and updated to prevent negative or unintended consequences to patients.
For more than 25 years, GalaxE Solutions has been a worldwide leader in providing creative and transformational technology solutions in Healthcare IT. Learn more about how GalaxE can transform your benefits management system and help you work smarter by going to https://galaxe.com/products today!